Product Details
What is this medicine used for?
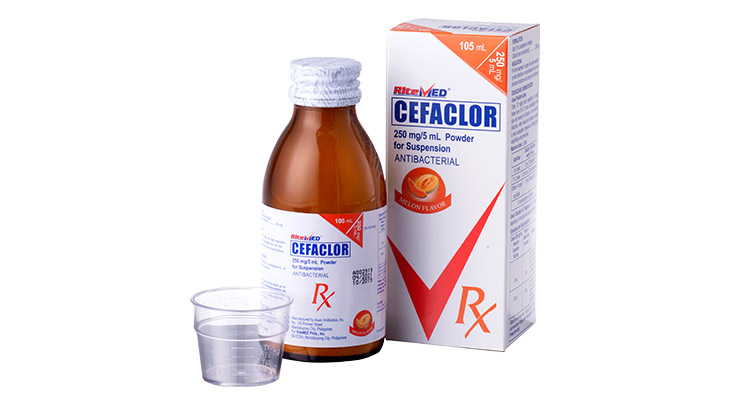
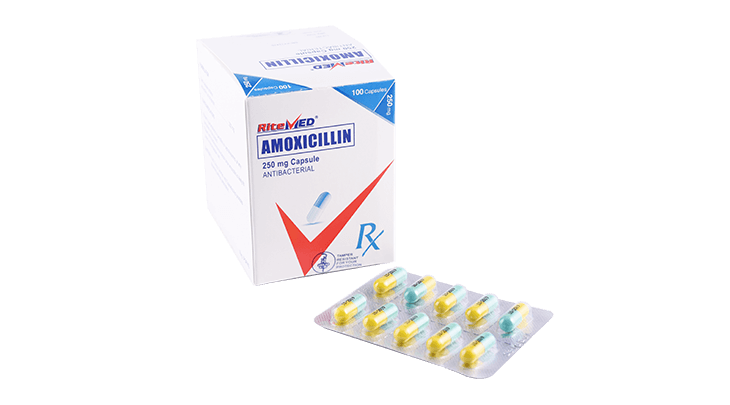
For the treatment of the following infections caused by susceptible microorganisms: Upper and lower respiratory tract infections including ear, nose, throat infections (e.g., acute otitis media). Gastrointestinal tract infections. Genitourinary tract infections. Skin and skin structure infections. Bone infections(e.g., osteomyelitis). Gall Bladder/ Biliary tract infections. Helicobacter pylori infections (in combination with other drugs) Lyme Disease. Dental abscess ( as an adjunct to surgical management). As prophylaxis for endocarditis: For the prevention of bacteremia, associated with p[rocedures such as dental extraction in patients at risk of developing bacterial endocarditis. Step down treatment for severe infections due to susceptible organisms, initially given intravenous antimicrobial therapy.
How much and how often should you use this medicine?
Usual Adult Dose: 250 mg to 500 mg every 8 hours or 500 mg every 12 hours, depending on the type and severity of infection. Maximum Dose: 6 g/day in divided doses. An adult dose of 3 g twice daily is recommended in appropriate cases for the treatment of severe or recurrent purulent respiratory tract infection. Usual Pediatric dose: Neonates and infants less than or equal to 3 months: 20 to 30 mg/kg body weight /day in divided doses every 12 hours. Infants >3 months and children <40 kg: 25 to 50 mg/kg body weight/day in divided doses every 8 hours or every 12 hours. Usual duration of treatment: For most infections: 5 to 14 days, depending on the type and severity of infection. Continue treatment for at least 48 to 72 hrs. after the patient becomes asymptomatic or after evidence of bacterial eradication has been continued. For beta-hemolytic streptococcal infections: at least 10 days to prevent rheumatic fever or glomerulonephritis. For Lyme disease: at least 12 days. Frequent bacteriologic and clinical appraisal is necessary during the treatment of chronic urinary tract infections and maybe required for several months after therapy has been completed.
Contraindication:
Known hypersensitivity to penicillins or cephalosporins, or any component of the product. Patients with infectious mononucleosis since amoxicillin is likely to cause a maculopapular rash.
Warnings and Precautions:
Serious and occasionally fatal hypersensitivity (anaphylactic) reactions have been reported in patients on penicillin therapy. These reactions are more likely to occur in individuals with history of penicillin hypersensitivity and/or hypersensitivity reactions to multiple allergens. Careful inquiry should be made concerning previous hypersensitivity to penicillins, cephalosporins or other drugs before initiating therapy with amoxicillin. If an allergic reaction occurs, the drug should be discontinued and appropriate therapy instituted. Serious anaphylactoid reactions require immediate treatment with epinephrine. Oxygen, intravenous steroids, and airway management, including intubation, should also be administered as indicated. Clostridium difficile-associated diarrhea (CDAD) and colitis have been reported with the use of nearly all antibacterial agents, including amoxicillin, and may range in severity from mild to life threatening. It is important to consider this diagnosis in patients who present with diarrhea following administration of antibacterial agents. During administration of high doses of amoxicillin, it is recommended to maintain adequate fluid intake and urinary output in order to reduce the possibility of cyrstalluria associated with amoxicillin therapy. In patients with renal impairment, the dose of amoxicillin should be adjusted based on the degree of impairment. As with any potent drug, periodic assessment of organ system function, including renal, hepatic, hematopoietic, is recommended during prolonged therapy. Prescribing amoxicillin in the absence of a proven or strongly suspected bacterial infection or a prophylactic indication is unlikely to provide benefit to the patient and increase the risk of the development of drug-resistant bacteria. As with other antibacterial drugs, long term or repeated use may result in overgrowth of non-susceptible organisms, including fungi.
Undesirable Effects:
As with other penicillins, it may be expected that untoward reactions will be related to sensitivity phenomena. They are more likely to occur in individuals who have previously demonstrated hypersensitivity to penicillins and cephalosporins and in those with a history of allergy, asthma, hay fever or urticaria. The following adverse reactions have been reported with the use of amoxicillin: Dermatologic/ Hypersensitivity reactions: Anaphylaxis, serum sickness-like reactions; severe allergic reactions including angioedema; exanthema, acute and generalized exanthematous pustulosis (AGEP), bullous and exfoliative dermatitis, erythematous maculopapular rashes, erythema multiforme, hypersensitivity vasculitis, mucocutaneous/oral and vaginal candiasis, pruritus, Stevens-Johnson syndrome, toxic epidermal necrolysis. GI: Nausea, vomiting, diarrhea, black ''hairy'' tongue, CDAD and colitis; hemorrhagic colitis; acute, transient enterocolitis with sever pain and bloody diarrhea, but without evidence of CDAD and colitis; glossitis, stomatitis, epigastric distress, gastritis, flatulence, soft stools, loss of appetite/anorexia, enanthemas/sore mouth or tongue, dry mouth, taste disturbances. Nervous system: agitation, anxiety, behavioral changes, confusion, convulsion, dizziness, reversible hyperactivity, hyperkinesia, insomnia. When penicillin reaches a high concentration in the CSF, neurotoxic symptoms consisting of myoclonia, convulsive seizures and depressed consciousness may occur. Unless drug administration is discontinued or its dosage reduced, the syndrome may progress to coma and death. Hemic and Lymphatic System: Anemia, including hemolytic anemia; agranulocytosis, abnormal platelet aggregation, eosinophilia, leukopenia, neutropenia, prolongation of bleeding time, prothrombin time and activated partial thromboplastin time(APTT); thrombocytopenia, thrombocytopenic purpura. Hepatic: A moderate rise in aspartate aminotransferase (AST) and/or alanine aminotransferase (ALT); transient increases in serum alkaline phosphatase and lactate dehydrogenase levels hepatic dysfunction including cholestatic jaundice. hepatic cholestasis and acute cytolytic hepatitis. Renal: Acute interstitial nephritis, crystalluria. Other Adverse effects: Tooth discoloration mostly pediatric patients. It most cases, discoloration was reduced or eliminated with brushing or dental cleaning.
Interaction w/ other medicaments:
Allopurinol: An increased incidince of skin rashes reportedly occurs in hyperuricemic patients who are concomitantly receiving allopurinol and amoxicillin receiving allopurinol and amoxicillin compared with those receiving amoxicillin or allopurinol alone. Anticoagulants: Prolongation of prothombromin time ha been reported rarely in patients receiving amoxicillin. Appropriate monitoring should be undertaken when anticoagulants are prescribed concomitantly. Bacteriostatic agenst (e.g., Chloramphenicol, macrolides, sulfonamides, and tetracyclines): these antibacterial agents with the bactericidal effects of penicillin. This has been demonstrated in vitro; however, the clinical significance of this interaction is not well documented. Beta-lactamase Inhibitors: in vitro and inin vivo studies indicate that the combination of amoxicillin with clavulanic acid or sulbactam results in synergistic bactericidal effect againts many strains of Beta-Lacatamase-producing bacteria. Digoxin: Concurrent administration with amoxicillin may result in increased absorption of digoxin. Methotrexate: Concomitant use of penicillins (e.g., amoxicillin) may decrease the renal clearance of methotrexate, presumably by inhibiting renal tubular secretion of the drug. Increased serum concentrations of methotrexate, resulting in GI or hemtologic toxicity, have been reported. Careful monitoring is recommended durng concomitant therapy. Oral Contraceptives: As the other antibiotics, amoxicillin may affect the gut flora, leading to lower estrogen reabsorption and reduced efficacy of combined oral estrogen/progesterone contraceptives. Probenecid: Concurrent use of amoxicillin and probenecid may result in increased and prolonged blood levels of amoxicillin. Interference with Laboratory Tests: High urine concentrations of ampicillin may result in false-positive reactions when testing for the presence of glucose in urine using Clinistest, Benedict's solution. Since the effect may also occur with amoxicillin, it is recommendedn that glucose tests based on enzymatic glucose oxidase reactions (e.g., Clinistix) be used. Administration of ampicillin to pregnant women may result in a transient decrease in plasma concentrations of total conjugated estrone, and estradiol. This effect may also occur with amoxicillin. Amoxicillin may interfere with protein testing when colorimetric methods are used.